Varicose veins are enlarged, twisted veins that most often appear in the legs. They develop when vein valves weaken and blood has a harder time flowing upward toward the heart. As pressure builds, veins stretch and become visible at the surface.
Many people seek care because of discomfort, swelling, or heaviness—but treatment can also help reduce the risk of complications related to poor circulation.
You may notice one or more of the following:
Call promptly if you have sudden, painful swelling, redness/warmth in one leg, a new hard tender cord-like vein, or any chest pain/shortness of breath.
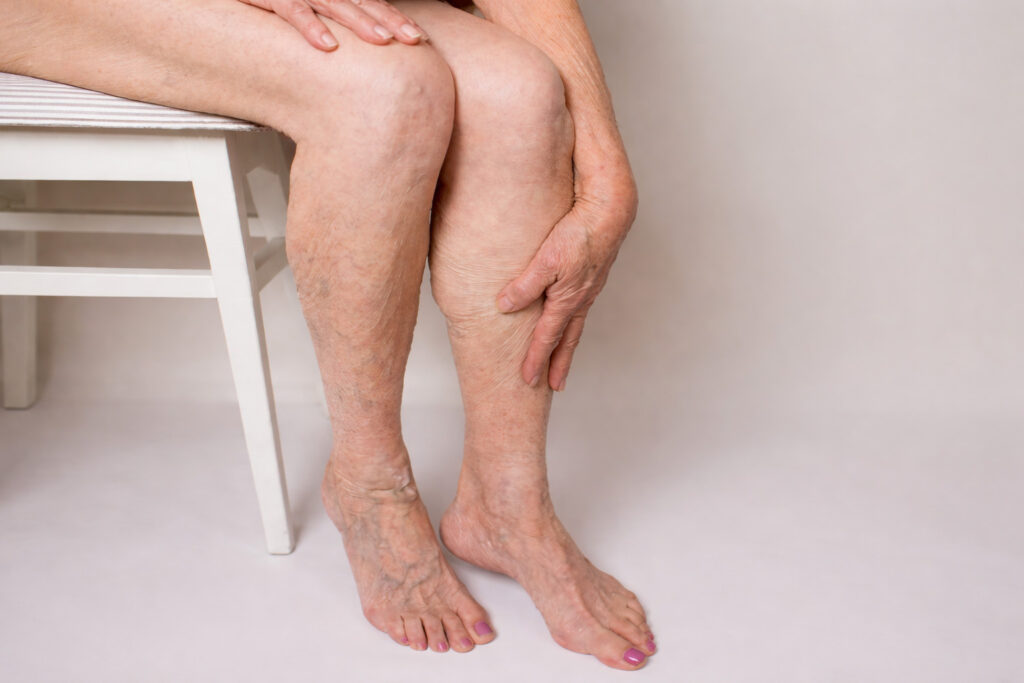
Varicose veins often develop from a combination of factors, including:
Varicose veins can range from mild to medically significant. Beyond appearance and discomfort, untreated vein disease may lead to:
A professional evaluation helps determine whether the issue is superficial, deeper valve reflux, or another circulation concern.
Varicose veins often reflect an underlying valve problem, not just what you see on the surface. Our evaluation is designed to identify the cause and guide the right treatment plan.
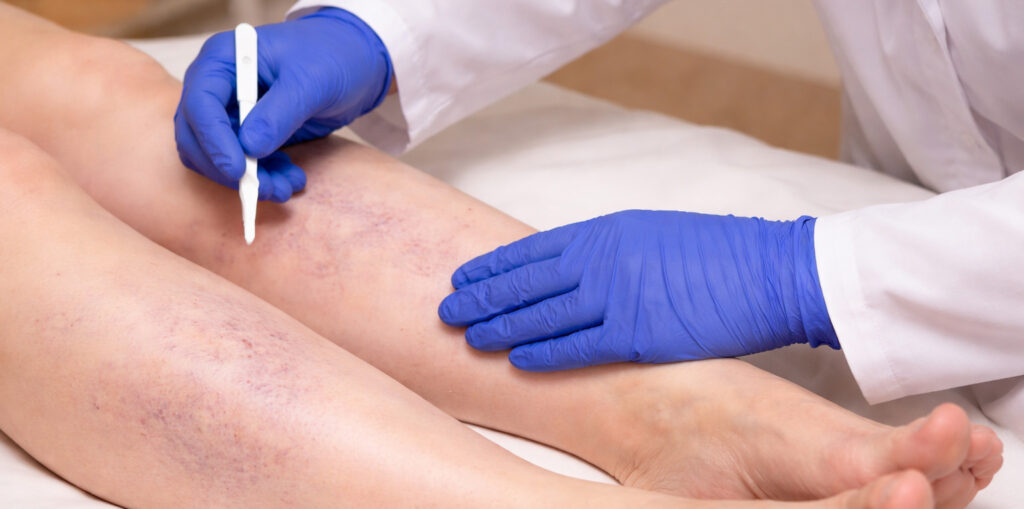
Below are six common options we may recommend, depending on your symptoms, vein size, and ultrasound findings:
A minimally invasive procedure that uses laser energy to close a refluxing vein from the inside, redirecting blood flow to healthier veins.
Similar to EVLT, this in-office treatment uses radiofrequency energy to gently seal the problem vein with local anesthesia.
A specialized foam solution is injected into targeted veins under ultrasound guidance to help close larger or deeper varicose branches.
Bulging surface veins are removed through tiny openings to reduce symptoms and improve appearance, typically with quick recovery.
Compression supports circulation, reduces swelling and heaviness, and is often used before and after procedures or for ongoing maintenance.
We recommend walking, leg elevation, movement breaks, and weight management strategies to reduce symptoms and help slow progression.